Global health impact and economic impact from the development of Freelite®
Submitting Institution
University of BirminghamUnit of Assessment
Clinical MedicineSummary Impact Type
TechnologicalResearch Subject Area(s)
Medical and Health Sciences: Cardiorespiratory Medicine and Haematology, Immunology, Oncology and Carcinogenesis
Summary of the impact
Research conducted by Professor Jo Bradwell at the University of
Birmingham provided the basis
of the commercially available diagnostic test Freelite®, which quantifies
free immunoglobulin light
chains in serum and was the first and only assay for the diagnosis and
monitoring of Multiple
Myeloma (MM). MM is a cancer of immunoglobulin producing plasma cells in
the bone marrow.
Freelite® has markedly improved the diagnosis and management of MM, is
helpful in the diagnosis
of all B cell lymphoid neoplasias and provides prognostic information for
premalignant conditions
present in over 3% of people over 50 years of age. Freelite was
commercialised by the University
of Birmingham spinout company, the Binding Site, which has achieved
worldwide sales, with over
360,000 tests being sold per month in 90 countries and an ongoing 25%
annual growth in sales.
The company provides annual revenue of £55m and employment for 620 people
in the UK and
abroad. An improved second generation of tests has been developed by
Professor Mark Drayson
at the University of Birmingham, which has been commercialised by a second
University spinout
company Serascience, which started marketing a point of care free light
chain diagnostic test
worldwide in April 2013.
Underpinning research
In the journal Lancet in 1847, Henry Bence Jones described the
characteristics of the first cancer
biomarker, a protein in urine from a patient who suffered with mollities
and fragilitas ossium
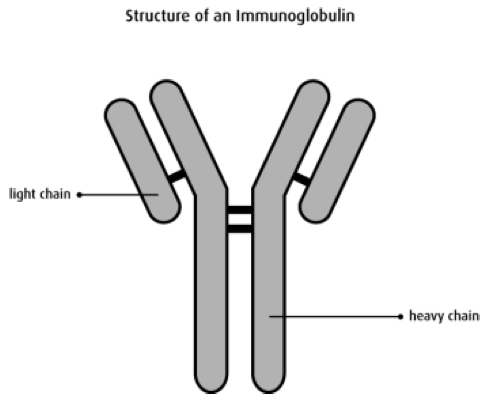
(myeloma). In the 1960s, the Bence Jones protein was identified as
immunoglobulin free light
chains (FLC), which when joined with the heavy chain make the whole
immunoglobulin complex
(see diagram below). FLCs and whole immunoglobulins are the products of
normal polyclonal
plasma cells (polyclonal immunoglobulin) and the neoplastic plasma cell
clone of myeloma
(monoclonal immunoglobulin — M-protein). Two forms of FLC are produced:
kappa and lambda,
with about twice as much being of the kappa type.
In healthy individuals the total body plasma cell pool produces about
0.5g/day of FLC, with a blood
half-life of 2 to 4 hours. FLCs are removed from the blood by filtration
into the kidneys and do not
appear in the urine of healthy individuals because they are metabolised in
the kidneys. In blood
cancers such as MM, a single plasma cell gives rise to a greatly expanded
neoplastic clone, which
will secrete FLCs of either kappa or lambda type; it is this
characteristic and the relative ratio of the
two FLC types, which the diagnostic tests described in this case study are
based. As a
consequence of the increased level of FLCs being produced in diseases such
as MM, the kidneys
become saturated and FLC become detectable in the urine. A neoplastic
clone of plasma cells
must secrete more than 20g of FLC per day (40x the combined secretion of
all the body's normal
polyclonal plasma cells) to saturate the kidneys and for FLCs to become
detectable in urine.
Accordingly, it is preferable to assess FLC secretion by measurement of
FLC in blood, not urine. A
neoplastic clone of plasma cells only has to secrete 1g/day of monoclonal
FLC to reveal its
presence by distorting the normal blood serum FLC (SFLC) kappa to lambda
ratio. Despite it
being preferable to measure FLCs in the serum, it was technically
challenging to develop such a
test, this is because the level of SFLCs is 1000 fold less than the level
of FLC in the bound form of
the whole immunoglobulin. Thus antibodies for the clinical detection of
SFLC must have a high
specificity for epitopes (areas which antibodies bind) that are exposed on
FLC, but are hidden on
the form bound to the heavy chain in the whole immunoglobulin. Furthermore
the FLC epitopes
that the diagnostic antibody recognises must be present on FLC from all
patients and normal and
neoplastic plasma cell clones.
In the late 1990s Professor Jo Bradwell, Senior Lecturer in the School of
Immunity and Infection at
the University of Birmingham (until September 2000) led a team to generate
polyclonal antibodies
in sheep for the development of laboratory assays to reliably quantitate
FLCs in serum samples [1].
The diagnostic test was based on unique sheep polyclonal antibodies
directed to either kappa or
lambda FLC, which were conjugated to latex beads. Following the addition
of FLC containing
serum sample to these antibody conjugated beads, turbidimetry or
nephelometry was used to
measure the amount of cross linked antibody, which was directly correlated
to the amount of
SFLC. Professors Bradwell and Drayson (UoB from 1991) used serum samples
from the national
MRC myeloma trials to validate the clinical utility of the test from 2000
onwards. The greater
sensitivity of measuring FLC in serum rather than urine was demonstrated
in myeloma patients
previously classed as non-secretory because the old gold standard methods
for detecting
monoclonal Immunoglobulin/FLC in serum and urine were negative [2].
Furthermore in myeloma
patients who secreted large amounts of FLC with no whole monoclonal
immunoglobulin detectable,
the new serum FLC test was shown to be greatly more sensitive for
detecting response to anti-myeloma
treatment and relapse from remission than the old urine Bence Jones
Protein test [3].
Prospective analysis of the SFLC test was made on 1,970 patients enrolled
into the MRC Myeloma
9 trial, confirming and furthering the findings of the retrospective
studies [4]. The results of this and
use of the SFLC test in the MERIT trial proved for the first time that
levels of nephrotoxic FLC could
be lowered quickly resulting in renal recovery and improved patient
survival and that the SFLC
tests provide an early and accurate measurement of disease response and of
relapse [5].
Despite the success of the original SFLC test, there are problems with
the reliance on polyclonal
antibodies which are difficult to produce and are very subject to batch to
batch variation. In
addition the sheep polyclonal antibody based tests (FreeliteTM)
are restricted to use on expensive
laboratory nephelometers and turbidimeters, have limited sensitivity and
range of FLC level
detection, along with antigen excess problems, where patients with
exceedingly high levels of
SFLC would be undetectable. The development of a second generation of FLC
tests based on use
of mouse monoclonal antibodies addresses the problems described above.
Professor Mark
Drayson led the development and clinical validation of the mouse monclonal
antibody based,
second generation SFLC tests over the last five years [6]. The use of
monoclonal rather than
polyclonal antibodies overcomes the long term problems of antibody
production and batch to batch
variation. Using competitive inhibition strategies overcomes the problem
of antigen excess and
greatly broadens the range of FLC levels that can be detected. The first
of these tests to be
described uses a flowcytometer platform with multiplexed beads enabling
kappa and lambda FLC
to be measured simultaneously, along with eight other immunoglobulin based
analytes. The
system has been adapted for nephelometry and turbidimetry platforms but
also ELISAs allowing
great flexibility on incorporation of the tests into different laboratory
systems worldwide.
Importantly the antibodies and the assay described above have been
integrated into a point of care
test which has been launched, bringing immediate improvement to patient
diagnosis and
management.
References to the research
1. Bradwell AR, Carr-Smith HD, Mead GP, Tang LX, Showell PJ,
Drayson MT, Drew R. Highly
sensitive, automated immunoassay for immunoglobulin free light chains in
serum and urine.
Clin Chem. 2001 Apr;47(4):673-80. PubMed PMID: 11274017.
2. Mark Drayson, Liang X. Tang, Roger Drew, Graham P. Mead, Hugh
Carr-Smith, and Arthur
R. Bradwell. Serum free light-chain measurements for identifying
and monitoring patients with
nonsecretory multiple myeloma. Blood 2001;97:9:2900-2902. DOI
10.1182/blood.V97.9.2900
3. Arthur R Bradwell, Hugh D Carr-Smith, Graham P Mead, Timothy C
Harvey, Mark T
Drayson. Serum test for assessment of patients with Bence Jones
myeloma. Lancet
2003;361:489-491. DOI 10.1016/S0140-6736(03)12457-9
4. Andy C. Rawstron, J. Anthony Child, Ruth M. de Tute, Faith E. Davies,
Walter M. Gregory,
Sue E. Bell, Alexander J. Szubert, Nuria Navarro-Coy, Mark T. Drayson,
Sylvia Feyler, Fiona
M. Ross, Gordon Cook, Graham H. Jackson, Gareth J. Morgan, and Roger G.
Owen. Minimal
Residual Disease Assessed by Multiparameter Flow Cytometry in Multiple
Myeloma: Impact
on Outcome in the Medical Research Council Myeloma IX Study. J Clin Oncol.
2013 Jul
10;31(20):2540-7. DOI: 10.1200/JCO.2012.46.2119
6. Campbell JP, Cobbold M, Wang Y, Goodall M, Bonney SL, Chamba A,
Birtwistle J, Plant T,
Afzal Z, Jefferis R, Drayson MT. Development of a highly-sensitive
multi-plex assay using
monoclonal antibodies for the simultaneous measurement of kappa and lambda
immunoglobulin free light chains in serum and urine. J Immunol Methods.
2013 Feb 3 . doi:
10.1016/j.jim.2013.01.014
Details of the impact
The development of the freelight chain assays by Professors Bradwell and
Drayson has had
significant impact on the clinical management of patients with B
cell lymphoid neoplasias and
has led to changes in clinical practice and commercial impact
through the success of the
Binding Site and the formation of Serascience.
Clinical impact
The SFLC test has been adopted into worldwide clinical practice because of
its importance in the
diagnosis and management of myeloma, solitary plasmacytoma and light chain
amyloidosis. This
is evidenced by numerous review papers, national and international
guidelines for the diagnosis
and management of these diseases [1]. These guidelines continue to be
updated as more
scientific evidence becomes available about the use of the test. The SFLC
test has been adopted
as a prognostic marker for the whole range of B lymphoid cancers and
premalignant conditions
including monoclonal gammopathy of undetermined significance which occur
in 3% of people aged
>60 years [2]. More recently it has been adopted as a prognostic marker
for survival in normal
populations [2]. Use of the SFLC test in the MERIT trial and in the MRC
Myeloma 11 trial has
made it clear that the SFLC response to the first few weeks of
anti-myeloma therapy reliably
predicts final response [3]; this allows early identification of
non-responders and change to a
treatment more likely to be effective in identified individuals.
Impact on patients
The ability to measure serum FLC levels has had a major impact on the
diagnosis and
management of all patients with plasma cell dycrasias and B lymphoid
lymphoma and leukaemia
[4]. In non-secretory and light chain only myeloma and in many
plasmacytoma and light chain
amyloid patients SFLC tests allow diagnosis and detection of changes in
disease activity that could
not be achieved before. The second generation of these tests
commercialised by Serascience is
making these tests more widely available, in particular a point of care
version, allowing patient
management decisions to be made more reliably and immediately in the
outpatient clinic, at the
bedside or even at home [5].
Commercial impact
The Binding Site was formed in 1982 by a group of researchers from the
University of Birmingham
Medical School, to manufacture and supply antibodies, alongside developing
a series of diagnostic
tests. Following the development of the SFLC test the Binding Site
incorporated the technology as
a key part of its product portfolio. In October 2009 the Binding Site sold
its autoimmune
diagnostics business to the Werfen Group SA, based in Barcelona, Spain for
£84 million in order to
concentrate on Freelite which accounted for most of its other annual
income and was growing at
40% per year [6]. The company's annual turnover in 2012 was £55 million
and the company
employs in excess of 550 people in the UK and abroad [7]. In 2012, 360,000
SFLC tests were sold
each month in 90 countries, directly through offices in UK, USA, Canada,
Germany, Austria,
France, Spain, Italy, Czech Republic, Slovak Republic, Belgium,
Netherlands and Luxembourg;
and through a network of over 70 distributors [7].
In 2010, the Binding Site won The Queen's Award for Enterprise in the
category International
Trade, for its outstanding achievement in increasing export revenues by
74% to over £42
million/year in 3 years and selling more than 90% of its production
overseas [8]. Aggregate
exports over this period totalled £96 million. This growth is primarily
driven by sales of Freelite®,
which has grown to £36 million/year in 2012 [7]. New jobs have been
created in sales, marketing,
research and clinical education, both in the UK and internationally, to
support this trade. In March
2011, the company moved its headquarters and 380 UK-based staff to larger
premises in the
centre of Birmingham. In April 2011 Nordic Capital Fund VII acquired the
Binding Site for an
undisclosed sum [9]. City analysts believe that sum to be in the region of
£200 million [10].
A new University spinout company, SeraScience, was formed in 2011 to
commercialise the
monoclonal based SFLC assay. The company was formed as a result of
significant investment
from the University and UK based Healthcare company, Abingdon Health. The
company has
successfully developed a new range of "point of care tests" for FLC, which
will mean that the SFLC
assay can be undertaken within the clinic, providing rapid clinical
assessment and immediate
information for the patient and clinical teams. The new range was launched
at the Biannual
International Myeloma Conference in Kyoto, Japan in April 2013 [11]. The
point of care test is
manufactured by FORSITE in Yorkshire (a spinout company from DEFRA). The
nephelometric and
turbidimetric assays are being developed with Spinreact in Gerona, Spain.
Sources to corroborate the impact
- International Myeloma Working Group guidelines for serum-free light
chain analysis in multiple
myeloma and related disorders, A Dispenzier1, R Kyle, G Merlini, JS
Miguel, H Ludwig, R
Hajek, A Palumbo, S Jagannath, J Blade, S Lonial, M Dimopoulos, R
Comenzo, H Einsele, B
Barlogie, K Anderson, M Gertz, JL Harousseau, M Attal, P Tosi, P
Sonneveld, M Boccadoro,
G Morgan, P Richardson, O Sezer, MV Mateos, M Cavo, D Joshua, I
Turesson, W Chen, K
Shimizu, R Powles, SV Rajkumar and BGM Durie on behalf of the
International Myeloma
Working Group. Leukemia (2009) 23, 215-224.
- Using Single Protein Biomarkers to Predict Health and Disease in
Diverse Patient Populations:
A New Role for Assessment of Immunoglobulin Free Light Chains. Mark T
Drayson, Mayo
Clinic Proceedings. Editorial June 2012;87(6):505-507.
-
Novel approaches
for reducing free light chains in patients with myeloma kidney. Hutchison
CA, Bladé J, Cockwell P, Cook M, Drayson M, Fermand JP,
Kastritis E, Kyle R, Leung N,
Pasquali S, Winearls C; International Kidney and Monoclonal Gammopathy
Research Group.
Nat Rev Nephrol. 2012 Feb 21;8(4):234-43. doi:
10.1038/nrneph.2012.14. Review.
-
www.myeloma.org.uk/index.php/download_file/view/2034/.
Myeloma Infoguide Series.
Serum Free Light. Chain Assay. Myeloma UK Serum Free Light
Chain Infoguide July
2012:6732 infoguide 25/07/2012 09:10 Page 1
- http://www.myeloma.org.uk/about-muk/news/myeloma-news/myeloma-uk-welcomes-new-diagnostic-test-for-myeloma/
- http://www.bindingsite.it/corporate-news?story=342
- http://www.thebindingsite.com/facts-and-figures
- http://www.thebindingsite.com/queens-award
- Nordic Capital Fund VII acquires diagnostics company The Binding Site — Press release, 14th
April, 2011 (http://www.nordiccapital.com/news/news-listing/nordic-capital-fund-vii-acquires-diagnostics-company-the-binding-site.aspx)
- Medical technology: Healthcare's third way
http://www.unquote.com/uk/analysis/2206565/medical-technology-healthcares-third-way
- http://www.serascience.com/